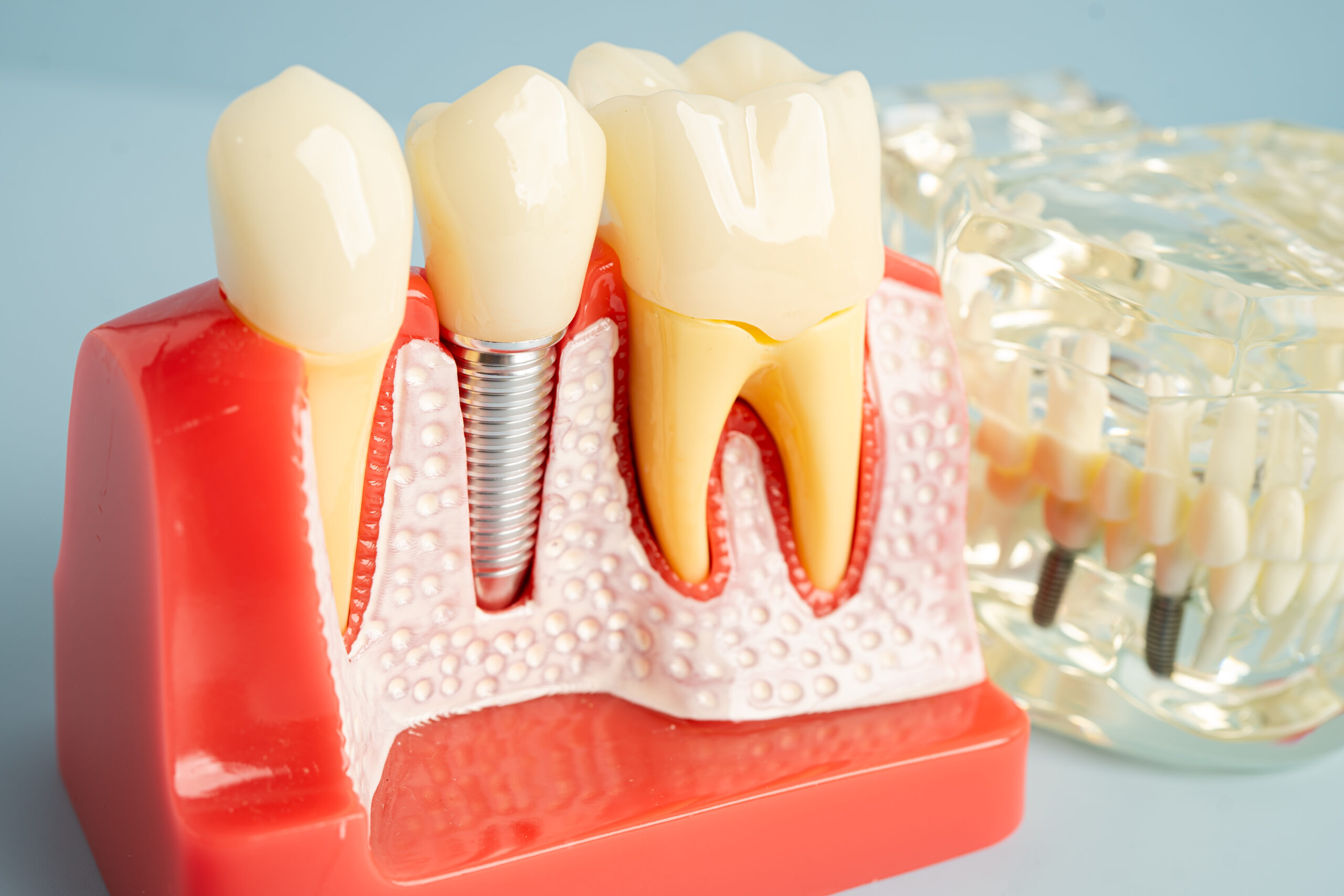
Dental implants are a top choice for replacing missing teeth. They restore your smile, improve chewing function, and last for decades when properly cared. But like any surgical procedure, they require your body to heal well. Certain health conditions can increase the risk of implant failure by negatively affecting this healing process.
In this blog, we’ll explore the connection between your medical history and dental implants to help you better prepare for a successful outcome.
Why Do Medical Conditions Matter for Dental Implants?
Osseointegration, the process of an implant fusing with your jawbone, is essential for a successful outcome. This healing process can be affected by anything that slows down tissue repair, weakens bone density, or disrupts the body’s immune response.
Certain health conditions don’t automatically disqualify you from getting dental implants—but they may require special planning, monitoring, or treatment adjustments. Being aware of how your medical history could play a role helps you and your dentist make informed decisions.
Common Medical Conditions That Increase Implant Failure Risk
Here are some of the most common conditions that may raise your risk of implant complications:
1. Uncontrolled Diabetes
Diabetes affects your body’s ability to heal and fight infection. If your blood sugar isn’t well-controlled, you face a much higher risk of implant failure. Poor healing can interfere with osseointegration, and higher glucose levels can promote bacterial growth around the implant site, leading to infection.
What You Can Do: If you have diabetes, managing your blood sugar is a key step in preparing for dental implant surgery. Talk to your primary care doctor and dentist about achieving stable blood sugar levels to reduce your implant failure risk.
2. Autoimmune Disorders
Conditions like rheumatoid arthritis, lupus, and multiple sclerosis involve an overactive immune response that can impact how the body heals. Some autoimmune medications also suppress the immune system, making infection more likely and slowing the integration of the implant with the bone.
What You Can Do: Let your dental team know about any autoimmune conditions or medications you’re taking. Pre-surgical planning and close monitoring after placement are essential.
3. Osteoporosis and Low Bone Density
Osteoporosis causes bones to become thinner and weaker over time, which can affect the stability of the implant post. Since implants rely on strong jawbone support, reduced bone density can make it difficult for them to anchor properly.
What You Can Do: A bone density scan or 3D dental imaging may be recommended before implant placement. In some cases, a bone graft can help build up the jawbone prior to surgery.
4. Cancer and Past Radiation Therapy
Patients who have undergone radiation therapy in the head or neck area may face a higher risk of implant complications. Radiation can damage blood vessels and reduce the bone’s ability to heal, especially in the jaw.
What You Can Do: If you have a history of cancer or radiation treatment, your dentist will evaluate whether dental implants are a safe option, and may consult with your oncologist if needed.
5. Heart Disease and Hypertension
While heart conditions don’t directly impact the implant site, they can affect your body’s overall healing ability and how well you respond to surgery. Certain heart medications may also increase bleeding or interfere with healing.
What You Can Do: Be sure to disclose your full medical history, including all medications. Your dentist may work with your physician to ensure safe treatment planning.
6. Smoking (Yes, It’s a Medical Risk)
Smoking is a major risk factor that dramatically raises the likelihood of implant failure. It restricts blood flow, slows down healing, and increases the risk of infection. Smokers also tend to experience more bone loss over time, which can compromise implant stability.
What You Can Do: If you smoke, quitting before and after implant surgery can significantly improve your chances of long-term success.
Can You Still Get Dental Implants If You Have a Medical Condition?
In many cases, yes. Having a medical condition doesn’t automatically mean you’re not a candidate for implants. But it does mean that extra care, communication, and planning are essential.
We may recommend:
- Pre-treatment screenings or blood work
- Bone grafting if bone volume is low
- Delaying the procedure until a condition is stabilized
- Specialized post-operative care or longer healing periods
Supporting Implant Success Through Better Health
If you’re living with a medical condition and considering dental implants, here are a few proactive steps you can take to protect your investment:
- Work with your physician to keep chronic conditions well-managed.
- Maintain excellent oral hygiene to reduce the risk of infection.
- Avoid tobacco products to promote healthy healing and bone support.
- Follow all pre- and post-op instructions from your dental team.
- Regular dental visits are important for monitoring the health of your implant and the nearby tissues.
Schedule Your Dental Implant Consultation in Wichita Falls Today
If you have a medical condition and are thinking about dental implants, the best first step is to schedule a personalized consultation. At Spearmint Dental & Orthodontics, we take the time to understand your medical history and create a treatment plan that supports long-term dental implant success.
We’ve helped many patients in Wichita Falls and the surrounding area safely move forward with dental implants, even with conditions like diabetes, osteoporosis, or heart disease.
Contact us to schedule your dental implant consultation and let our team guide you through the next steps with care and clarity.